|
The claims then undergo an in-network review, where the doctor and facility are checked to confirm if they are in-network based on the patient’s insurance plan. The next check involves verifying the patient’s insurance coverage at the time of service. The first is an initial review, which ensures that there are no spelling errors, dates are correct, and there are no duplicate charges. Initial Reviewīefore the claims are processed, they undergo several checks. 
Electronic claims, on the other hand, are directly entered into the system. Paper claims are either scanned or manually entered into the system. This can be done either electronically or via traditional paper mail. When a patient visits a clinic or healthcare provider, the appointment and services rendered are documented and submitted for reimbursement from the insurance company. This section explores the steps involved in the process. Generally, the journey of a medical claim involves much human effort and many time-consuming processes. Automation solution makes this information-intensive process to be more organized driving organizations to find paths to improve their customer experience within their revenue margin. Processing medical claims is a crucial aspect of the healthcare industry that involves submitting and managing claims for medical services rendered to patients. The processing time will depend on the complexities of the medical services rendered and the denials encountered and how organizations effectively collect a patient’s details.Īn intricate understanding of the fundamentals of claims processing will benefit healthcare providers with a smooth revenue cycle and allow quality healthcare.The provider then must resubmit the claim with the requested changes. If the claim is incomplete or incorrect, the insurance carrier will send the claim back to the provider for additional information or correction.Enough steps to ensure all the checkpoints are met, and the insurance company will reimburse you for the payment.The data is collected by medical staff, such as physicians, nurses, and medical technicians, and then submitted to the insurance provider.This includes a variety of data points such as the patient’s name, address, date of birth, insurance information, and diagnostic codes. Typically begins with the patient’s medical record and ends when the healthcare provider receives full reimbursement for all the services delivered to the patients.Collecting, validating, and processing data from various sources to ensure that patients receive the correct care and are reimbursed for the services they receive.The fundamentals of a medical claims workflow process involve: 
A claims processing workflow helps to streamline the insurance industry’s most challenging claims process and protects the organization against reputational damage. The medical claim processing workflow is the set of steps that medical staff and insurance companies must take to ensure accurate and timely reimbursement to the patient. Without medical claims, healthcare providers wouldn’t be able to bill for the services they provide and patients wouldn’t be able to receive reimbursement from their insurance companies. 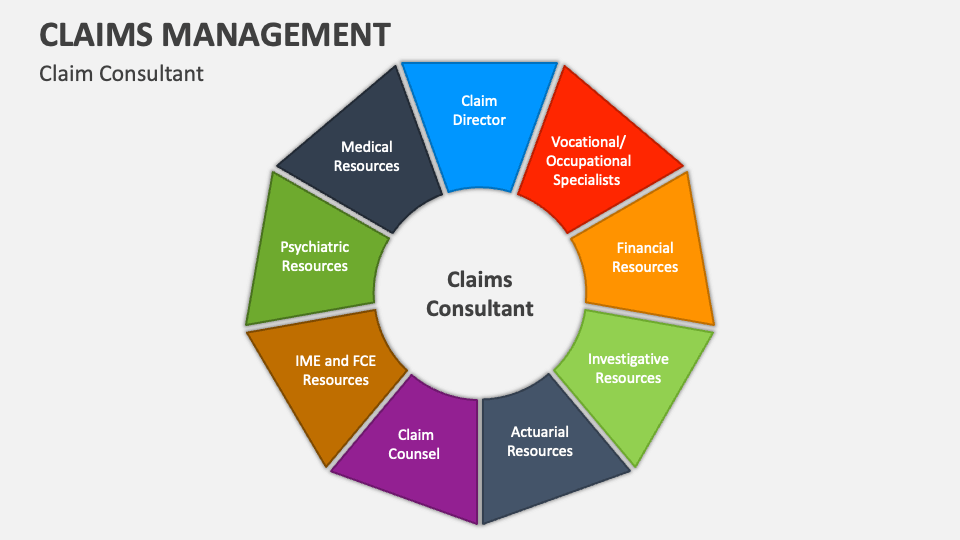
A medical claim typically includes the patient’s name, date of service, procedure code, diagnosis code, and the provider’s name, address, and National Provider Identifier (NPI) number.Īdditionally, medical claims also include the patient’s policy information, the cost of the service, and the amount being charged. Medical claims are invoice documents that are submitted to insurance companies to request payment for services rendered by a healthcare provider. Medical claims are an important part of the healthcare industry. This blog also lists the importance of claims processing workflow in the healthcare industry and the best practices involved in unraveling the mysterious claims processing. This write-up explores the journey of the medical claim and the challenges involved in claims processing. Creating a better claims process requires a comprehensive understanding of the customer experience, a commitment to continuous improvement, and a willingness to embrace new technologies. A McKinsey study reveals that “ By 2025, around 25% of the insurance industry is expected to use automation workflows for processing claims, underwriting tasks, and other insurance filing activities”.Īre healthcare providers aware of what is essential to accelerate organizational efficiency and enhance customer experience?- The answer would be surprising and it is a better-processed claim! What is an ideal solution to achieve it? A claims processing workflow!Ī well-managed claims process ensures that customers can quickly and easily receive the compensation they are entitled to.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
